Diastasis Recti: Why It's Not As Scary As It Sounds

by Team Thinx
What's the Lowdown on Diastasis Recti? (let's just call it DR, shall we?)
Some call DR "Mummy Tummy," but honestly, we'd rather not because it kinda makes us cringe. Let's be real, everyone has a stomach and there's no need to sugarcoat this postpartum condition by giving it an overly cutesy name just because we're referring to new moms. When you're growing a human inside of you, your stomach muscles stretch, and that is truly miraculous. (Sidenote: Why are "Dad Bods" all the rave? #TeamMomBod 🤔)
Ok, so what is DR? To orient us, Lindsey, our resident pelvic floor therapist & women's health extraordinaire, explained it to us. DR affects our inner and outer core, which is made up of:
the rectus abdominis (what we call our abs)
the linea alba (the middle piece that vertically connects both sides of our abs)
the internal and external obliques (those things on the side)
the transversus abdominis (the deepest core muscle layer under it all)
the pelvic floor
diaphragm
the multifudius muscles (your back support)
Keep in mind, because your bulbous belly is growing and accommodating for a wee (or giant) bub(s), the muscles must expaaaaaand. Typically, this means that most pregnant women experience DR to some extent around the third trimester. When the widening happens, Lindsey explained, the linea alba (that vertical midline tissue) can't contract or connect all the core muscles. "Most abdomens recover after birth, and the midline will eventually return to its functional state," she said. "But some women continue to experience DR in the postpartum period for as long as a year after birth."
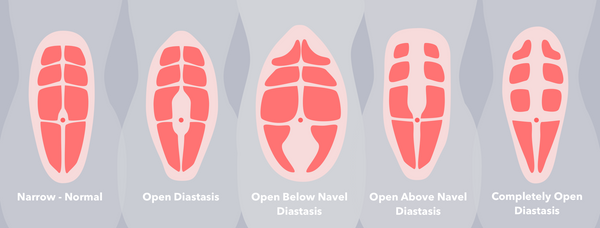
Imagine if you're stretching out dough (mmm...fresh bread), the unbaked goodness will expand and get thinner until it eventually separates into two pieces. To put it visually, your six-pack muscles becomes 2 three-packs if you've got DR.
If untreated, DR can wreak havoc on your bod & its functions and even cause leakage or pelvic organ prolapse. Our abs are deeply connected to the pelvic floor muscles through the fascial system. And sure, while the exterior of our stomachs get the most attention, our interior muscles are actually the real MVP (Most Valuable Parts 😉); they help support the pelvic lumbar, hip girdle region, and hold reproductive organs and intestines in place.
But Yeah, Are There Symptoms?
So how can you tell if your core muscles have separated and are a little unwilling to meet in the middle? During pregnancy, Lindsey suggests women see a physiotherapist to have core strength assessed. Getting checked for DR is more informative postpartum. Most women visit pelvic floor therapists like Lindsey in the weeks, months, and in many cases years, after delivering a baby. They notice signs like:
a protruding belly
general feeling of weakness in their core
incontinence that continues more than 8 weeks postpartum
constipation
gassy and bloating after meals
pain during intercourse
lower back pain
How To Check Yourself For DR
Because Lindsey is a real-life health goddess, she kindly put together this video to demo how women can check themselves for DR.
Lie flat on your back with your feet on the floor and knees bent toward the ceiling.
Put your fingers right above your belly button and press down gently.
Then lift up your head about an inch while keeping your shoulders on the ground.
If you have DR, you will feel a gap between the muscles that is wider than an inch. More telling, however, do your fingers sink down into your stomach? If there's no tension when you contract your core or it feels gooey, get it checked out.
Lindsey says that historically, DR has been diagnosed when there's a gap of 3 fingers or more between the core muscles. Now, because of high-tech advances like internal ultrasound imaging, she says health pros can study what's going on inside. Recent research shows that it’s not so much about bringing the gap back together. Rehabilitating the deep core system will restore the integrity in your pelvic floor, transversus abdominis, diaphragm, the multifidus muscles of your back.
Irene Donahue, a postnatal fitness specialist whose forte is core restoration, agrees. When Irene's son was 3, she learned that she had pelvic organ prolapse. She was shocked to find out that the way she had been exercising (with faulty breathing mechanics, poor alignment, and excessive emphasis on her external abs) had been a huge contributing factor.
After healing and getting educated on pelvic health therapy, Irene now helps women who were in the same position as she was postpartum. Take for instance, Evi, a 38-year-old mom of 3 who didn't know anything about DR after delivering twins—that is, until she saw Irene's flyer at a doctor's office. Evi was itching to get back to CrossFit, but when she started working with Irene, she learned that patience and persistence is key to recovery. Irene says that her training programs are unique because no two women (or bodies) are exactly the same.
In case prolapse or pelvic floor dysfunction is present, Irene encourages for every mom to at least have an assessment with a women's health pelvic therapist like Lindsey. (Don't know how to find someone like Lindsey? Check this out.). "My clients who do some pelvic floor PT in conjunction with my functional exercise training program always have the best results," she shared.
Thankfully, Evi caught her DR before it caused any leakage or troubles with her pelvic floor. "If you ignore it or work out like crazy, you might be making it worse. You might need surgery or end up having a much bigger problem," Evi told me. "When life's busy and crazy, that's really the most important time to listen to your body." Essentially, she said, prioritizing your own health means you're being a stellar role model for your kids.
If You Have DR, What's Next?
Up until recently, rehab specialists have focused on rapid-style crunches or intensive ab workouts. Lindsey said that some preach this method in hopes of closing the vertical gap. But in reality, doing too many sets of traditional crunches can actually exacerbate DR because it further strains the core. As Lindsey and Irene mentioned, whether you're 29 or 79, it's never too late to fix your DR. Here are some of the Dos and Don'ts:
DO find a pelvic floor therapist and fitness expert you trust. These pros understand that the internal work is where longterm healing happens. Most importantly, they can tailor recovery to your specific DR needs.
DON'T hold your breath because it strains the linea alba (remember, that's the connective tissue that holds the recti abdominal muscles together) and your pelvic floor muscles.
DON'T do a gazillion crunches, intensive ab workouts, or jump into an exercise routine without seeking help from a fitness expert or pelvic floor therapist.
DO address any scar tissue if you've had a C-section, myomectomy, hysterectomy, or a laproscopic procedure. It can prevent DR from closing. Here's a scar care guide and video Lindsey put together!
DO eat well. Studies show that proper nutrition can aid with muscle repair. Grass-fed collagen, for instance, is a great supplement to include in your morning smoothie.
DO take a look at this free resource a la Lindsey on caring for your bod.
Don't forget, there's no magic remedy and the healing process isn't one-size fits all. Like everything worth working for life, patience is key. 🙏🏾
~*Learn more about Lindsey’s work and her free guides & videos. What health condition(s) do you want us to investigate next? 🔍 Comment below or write a note to natalie@shethinx.com!*~
Posted: July 31, 2019
Related Articles
one new subscriber wins a free pair of Thinx every day! see rules


